We experience stress throughout our lives when switching jobs, buying homes, or other major life changes. Though these events cause short-term concerns, they don’t usually do much damage. Chronic stress is more severe, resulting from long-term issues, like financial strains or life-altering medical conditions. When combining stress and arthritis, your symptoms often worsen, increasing joint pain and reducing quality of life.
Rehab for arthritis offers the proper treatments to cope with those overwhelming symptoms. It includes physical therapy, featuring safe exercises to improve muscle support and range of motion in your arthritic joints. Therapy may also include treatment for neurological diseases related to high stress levels that contribute to arthritis pain. To learn more about the relationship between chronic stress and joint pain, keep reading.
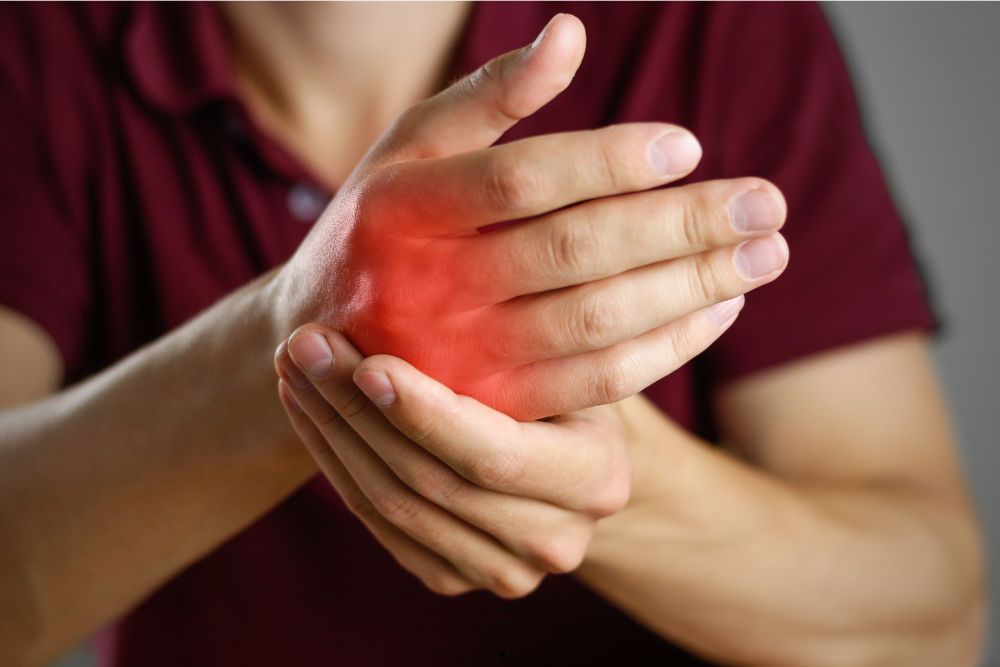
Is there Any Connection Between Stress and Arthritis?
Yes, even your thoughts, emotions and stress can influence your perception of pain, including joint pain. Stress, anxiety, and negative emotions can exacerbate pain by increasing muscle tension and releasing stress hormones like cortisol, which can heighten sensitivity to pain.
The pain, inflammation, and reduced range of motion of arthritis limit your ability to perform your usual daily tasks. Losing independence causes higher stress levels, affecting your joints, muscles, and immune system. The symptoms become more prominent, creating a vicious cycle of stress and arthritis pain. The following sections cover the worst offenders related to chronic stress and the damage it does.
Tense muscles
The body reacts to stress by increasing tension in every muscle. When the situation calms again, those muscles all relax. Though we’re designed to withstand short spurts of distress, our bodies can’t handle chronic stress. It’s especially damaging for those with arthritis or other medical conditions.
When our bodies are on alert for long periods, those tense muscles increase pressure on arthritic joints. The tension increases pain, which then causes more stress and even more pain. Though it’s impossible to avoid all stressors, learning coping methods is essential to breaking that cycle. Calming the mind and body reduces the tension and eases the pain.
Inflammation
When you’re dealing with chronic stress, the opposite occurs. Those hormones alter the immune system, increasing inflammation and causing issues with several medical conditions. For those with arthritis, the higher the swelling in those joints, the more pain you experience. The longer you’re under stress, the more inflamed the joint and arthritis gets, and the more discomfort you’ll suffer from.
Short bursts of tension release hormones triggering the fight or flight response. Some of those hormones also reduce inflammation in the body. As stress levels decrease, the body slows the release of those hormones, returning the body to its initial pre-stress state.
Stress and immune system
As we mentioned above, stressful situations release hormones that trigger an immune response. The reaction is the body’s way of preventing damage to the body’s delicate systems. For short periods, the immune system does its job, keeping you safe from harm.
When dealing with chronic stress and arthritis, the immune system has a negative reaction. Those hormones alter the immune response, attacking healthy tissue instead of protecting it. In fact, studies have shown that in some cases, chronic stress increases the risk of inflammatory arthritis, including rheumatoid arthritis. So not only does chronic stress worsen existing symptoms, but it may also cause the issue long before you notice any damage.
The connection between stress and the immune system is intricate. Your body’s defense mechanism can detect when you’re experiencing stress related to work, family, finances, or current events. The immune system is particularly responsive to psychological stress, particularly if it persists over time.
Long-term stress can lead to elevated levels of cortisol, disrupting the body’s ability to combat inflammation and potentially resulting in recurrent infections, as indicated by recent studies in immunology.
Both chronic stress and disruptions in the immune system can contribute to the development and exacerbation of arthritis. Therefore, managing stress levels and supporting immune system health are important aspects of managing arthritis and reducing its impact on daily life.
Resources:
- Arthritis Foundation, How stress affects arthritis https://www.arthritis.org/health-wellness/healthy-living/emotional-well-being/stress-management/how-stress-affects-arthritis
- American Psychological Association, March 8, 2023, Stress effects on the body https://www.apa.org/topics/stress/body
- Yun-Zi Liu, Yun-Xia Wang, and Chun-Lei Jiang, June 20, 2017, Inflammation: The common pathway of stress-related diseases https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5476783/
- 1, 2021, Perceived stress and inflammatory arthritis: a prospective investigation in the studies of the etiologies of rheumatoid arthritis (SERA) cohort https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7145743/
- How Does Stress Affect the Immune System? Stress and Immune System Function https://health.umms.org/2020/11/10/stress-immune-system/#:~:text=Stress%20and%20Immune%20System%20Function,to%20the%20American%20Psychological%20Association.
This content comprises informative and educational resources only and can not be considered as a substitute for professional health or medical guidance. Reliance on any information provided in this article is solely at your own risk. If you have any inquiries or apprehensions about your medical condition or health goals, talk with a licensed physician or healthcare provider.






Leave A Comment